Dr. John T. McDevitt saw the coronavirus coming. His wife, Anna Grassini, had been hearing about Covid-19 from her family in Italy since February. She recalls one message from her brother about a newspaper in a small town northeast of Milan whose obituaries spanned 10 pages; they usually took up two. It was like a horror movie, she said.
Over the last 10 years, McDevitt, chairman of the Department of Biomaterials and Biometrics at NYU’s School of Dentistry, has developed a cardiac scorecard — a tool to predict cardiac disease outcomes — with his team at the McDevitt Research Lab. The scorecard, currently in line for commercial release, uses certain biomarkers, or “internal disease thermometers,” that can indicate whether someone is more likely to have a severe case of the disease. T
Amid rising coronavirus cases, McDevitt wondered if he could take that research and use it to develop a similar model for Covid-19. During a regular team meeting on March 13, that’s exactly what he proposed. The result is a “risk-assessment tool” that lives inside of a phone app for clinician use.
While other groups have developed a way to determine how likely someone is to contract the virus, McDevitt’s app is unique in that it will help clinicians show patients just how bad their case will be — all from just one (or two) drops of blood that are measured on site and sent off to a lab. The number, between 0 and 100, shows a person’s probability of dying based on data like sex and age alongside four specific biomarkers for Covid-19 which, if present, can determine how severe the case will be. One of them, cardiac troponin I, is the biomarker for cardiac disease.
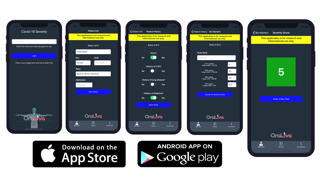
Digital rendering of the app. (Photo courtesy of Dr. John T. McDevitt.)
Scientific papers usually take four to six months, according to McDevitt. But given the escalating cases in New York at the start of March, he and lead author and algorithm developer Dr. Michael McRae, who also developed the algorithm for the cardiac scorecard as a part of his 2016 PhD dissertation, knew they had to work faster. Without access to their lab, the team had to turn to any and all scientific papers on coronavirus. Before their paper was submitted on April 10, they read through over 200 papers — many of which hadn’t even passed the peer review process yet. On April 7, Dr. Zhibing Lu of Zhongnan Hospital of Wuhan University reached out saying that he had data to share from 160 patients. McRae, who had already finished the paper by then, effectively re-wrote it in the four days leading up to the April 10 deadline.

Dr. McDevitt (top left) and his team. (Photo courtesy Dr. John T. McDevitt)
But this was only the start of April. After cases peaked in New York, the team knew they could get data from hospitals in the city. Enter Dr. Isaac Dapkins of NYU Langone, the university’s network of family health clinics that tend mostly to underserved communities and individuals who can’t afford insurance.
Dapkins had lost an older patient to Covid-19 in early April. During a telehealth visit that month, Dapkins found that the older Latinx man had symptoms consistent with Covid-19. But the man was afraid to go to the emergency room. He got sicker and by the time he made it to the hospital, it was too late.
This case further stressed the importance of a risk-assessment tool for Dapkins. He needed a concrete way to determine who was most at risk in order to know how to follow up with those patients. If Dapkins had had a severity score for that April patient, he could’ve known how fast he needed to check up with him. Possibly, he could’ve saved his life.
Now Dapkins is providing the McDevitt team with data from NYU Langone patients. The app is still being finalized, but has already been tested on a couple of people.
While the team’s first paper was based on data from the 160 Wuhan patients, the second (which the team is currently working on and will submit soon) will be trained on data from 1,236 NYU Langone patients. Having this fresh, New York-based data will allow the team to test their Wuhan-based algorithm and see if it can be generalized to New York City and beyond.
Informing patients of their risk is a challenge, especially those in minoritized communities who are more likely to distrust medical and government officials due to systemic lack of access to healthcare and lack of sufficient benefits in their jobs, according to Rachael Piltch-Loeb, a postdoctoral preparedness fellow at the Harvard TH Chan School of Public Health.
Given that NYU Langone’s network of family health centers is 39 percent Latinx or Hispanic and 51 percent non-Hispanic with 18 percent of those identifying as Black or African American, this is a major concern. And, Dapkins notes, those populations are more likely to see higher rates of hypertension and diabetes, both risk factors for the disease.
Generally, people are more likely to trust those within their community for risk information rather than a doctor or other authority figure they don’t know, Dr. Piltch-Loeb explained. This is especially evident in those underserved communities who are already feeling distrustful. (In the future, McDevitt’s team plans to incorporate race into the app’s algorithm to determine how it could impact the score.)
It also comes down to people’s individual perceptions — what they feel is putting them in danger rather than what actually is.
“Things that are further away seem less of a concern to us,” Piltch-Loeb said.
Dapkins agrees. “If people are careful, they will protect themselves but if you don’t believe that that’s actually valuable then you are going to get the virus at a higher rate,” Dapkins explains, “That’s a fact, there’s nothing else to that.”
The app can’t fix this human tendency. One of the surest ways to help people understand their individual risk is by having consistent messaging across federal and state governments. This is something that, as Piltch-Loeb notes, the U.S. has failed to do. The other part is developing trust between patients and providers. In other words, it’s important to not only make an app that works, but to ensure the clinicians using the app are doing so in a meaningful way.
“It has a lot to do with trust and then again, familiarity that’s developed by having had that personal interaction,” Piltch-Loeb said.
In the future, NYU Langone center clinicians will develop a protocol during appointments where, once the clinician has received the score, they’ll know exactly how to communicate that score to the patient and let them know when and how they’ll follow-up. Dapkins hopes that all of this will be fully up and running if or when New York experiences a second wave.
So far, McDevitt’s team says the app is working. “The signatures found, initially in Wuhan, are translatable into New York City and vice versa,” McDevitt said. McRae said that their second paper has equal, if not better, diagnostic accuracy than the algorithm for the app they developed in the first. Later, the team hopes to have the app take and process a patient’s blood sample and produce a score all within a single visit.
And Dapkins says that there’s been hope at Sunset Park, the NYU Langone clinic that is acting as its testing site. As of June 17, the Sunset Park clinic had just 40 or so patients hospitalized for Covid-19. On any given day in April, they had around 400. Dapkins also said that through testing they’ve found that about half of their Brooklyn patients have antibodies that could indicate a possibility for immunity.
Regardless, Piltch-Loeb, Dapkins, and McDevitt all agree: Covid-19 is here to stay. This app could be critical in helping doctors and clinicians better determine how to reach those that are most vulnerable.
“This is probably the challenge of our lifetime.” McDevitt said of Covid-19, “It’s lasting through the summer, it’s lasting through the hot months, it’ll be here through the fall.”